⚡ Quick Answer: At the correct dose (17 g/day), MiraLax does not typically cause cramping. Cramping can happen if you take too much, are dehydrated, have IBS, or have an underlying gut problem. Keep reading to understand exactly when and why — and what to do about it.
If you’ve ever stood in the pharmacy aisle wondering, “does MiraLax cause cramping?” — you’re not alone. MiraLax is one of the most widely used laxatives in the United States, yet many people are confused about its side effects, especially abdominal cramps and discomfort.
This guide covers everything: how MiraLax works in plain language, when cramping happens and why, how it compares to every major OTC laxative, the correct dosage for adults and children, drug interactions, colonoscopy prep, overdose guidance, storage tips, and the latest clinical evidence — with up-to-date 2023 AGA-ACG Joint Guideline evidence grades throughout.
📚 Related Reading on Constipation Relief:
1. What Is MiraLax?
MiraLax is the brand name for polyethylene glycol 3350 (PEG 3350) — a type of laxative called an osmotic laxative. It comes as a white powder that is tasteless, grit-free, and dissolves completely in any hot or cold drink.
Key facts at a glance:
- FDA-approved as a prescription drug: February 18, 1999 (NDA 20-698, submitted by Braintree Laboratories)
- FDA-approved for over-the-counter (OTC) sale: October 6, 2006 (NDA 22-015); available at retail stores from early 2007
- Currently marketed by Bayer Consumer Health (a division of Bayer AG)
- Each dose = 17 grams — no sugar, no preservatives, no gluten
- Available as: powder bottle, single-use packets, and flavored versions
2. How MiraLax Works
MiraLax is an osmotic laxative. Here is exactly what happens when you take it:
- You stir the powder into a drink and swallow it
- The PEG 3350 molecules travel into your intestines
- They form bonds with water molecules, trapping water in your stool instead of letting the colon absorb it back into your body
- Your stool becomes softer, wetter, and easier to pass
- The bulkier stool gently triggers your colon’s own natural muscle movements (called peristalsis)
- Result: a soft, comfortable bowel movement — usually within 1 to 3 days
What makes MiraLax different from most laxatives:
- ✅ Not absorbed into your bloodstream — stays entirely in your gut
- ✅ Not broken down by gut bacteria — no gas is produced
- ✅ Does not stimulate or irritate the nerves in your colon wall — no forced contractions, which means no cramping
“PEG forms hydrogen bonds with water molecules. For this reason, it can prevent the reabsorption of water, which causes water retention in the stool and increases the osmotic pressure. As a result, the stool softens, and bowel movements occur more frequently.” — Hammer HF. StatPearls, National Library of Medicine (NBK557652)
These three words describe the same single process: osmosis. In medical literature, PEG 3350 has one mechanism of action. The three-step marketing description is a simplified consumer-friendly way to explain one thing.
🟢 MiraLax Original 30-Dose Bottle
Standard polyethylene glycol (PEG 3350) powder for gentle constipation relief.
👉 Check Price on Amazon💰 Amazon Basic Care ClearLax (Generic PEG 3350)
Same active ingredient as MiraLax at a lower cost.
👉 View on Amazon🎒 MiraLax Single-Use Packets (24 Count)
Pre-measured doses — perfect for travel or work use.
👉 Buy Packets on Amazon🌿 Magnesium Citrate Powder (Natural Option)
Faster-acting osmotic alternative for occasional constipation.
👉 See on iHerb
3. Does MiraLax Cause Cramping?
✅ No — at the correct dose of 17 g per day, MiraLax does not typically cause cramping.
Here is what the clinical research actually shows:
- A 2016 placebo-controlled trial (Joo et al., World J Gastroenterol, PMC4848251) found that PEG 3350 increased bowel movements while also reducing cramping and gas compared to where patients started.
- A 2011 review of 21 clinical trials covering 1,949 patients (Zurad & Johanson, Curr Med Res Opin, PMID 21604961) concluded that PEG 3350 has “a safety profile comparable to that of placebo.”
⚠️ Transparency note: This review was funded by Bayer US LLC (the company that sells MiraLax). Its conclusions were independently confirmed by the 2023 AGA-ACG guideline, which was not funded by Bayer.
- The 2023 AGA-ACG Joint Clinical Practice Guideline (Chang et al., Gastroenterology, 2023) gave PEG the only strong recommendation for chronic OTC use among all laxatives reviewed — based on moderate certainty of evidence.
- The FDA drug label for MiraLax specifically states it does not cause “harsh side effects such as gas, bloating, cramping or sudden urgency” at the standard dose.
That said: “usually doesn’t cause cramping” does not mean “never.” A minority of users do experience cramping. The 6 main reasons are explained in the next section.
4. Six Reasons MiraLax Can Cause Cramping
Reason 1: You’re Taking Too Much (the Most Common Cause)
More than 17 g/day draws more water into the colon than it can handle comfortably. This causes pressure, bloating, and cramping. Taking extra does not make it work faster — it just causes pain and diarrhea. Stick to the recommended dose.
Reason 2: You Already Have Bloating or Gas
If you take MiraLax when you already have a lot of gas or bloating — common with IBS-C or SIBO — the extra fluid can temporarily make discomfort worse before things improve. This is not a true drug reaction. It is your bowel adjusting to more movement in an already-sensitive gut.
Reason 3: You Have IBS (An Important Distinction)
People with irritable bowel syndrome (IBS) have a more sensitive gut. Even a standard dose of MiraLax can trigger discomfort in IBS patients. Importantly, the 2023 AGA-ACG guideline’s strong evidence for PEG is for Chronic Idiopathic Constipation (CIC) — not specifically for IBS-C. The drug label says: “Ask a doctor before use if you have irritable bowel syndrome.”
Reason 4: You Are Dehydrated
MiraLax draws water from your gut into the stool. If you’re already low on fluids, this shift can cause cramping. Drink at least 8 glasses (64 oz) of water per day while taking MiraLax. Staying well hydrated also makes MiraLax work faster and more smoothly.
Reason 5: You’ve Been Using It Too Long Without a Doctor
The OTC label limits use to 7 days without medical supervision. Using it longer without guidance can change how your gut functions, leading to increased sensitivity and discomfort. If you need a laxative for more than a week, see a doctor to find out why.
Reason 6: A Serious Gut Problem May Be Present
⚠ Stop MiraLax right away and see a doctor if:
- Cramping is getting worse, not better
- You see blood in your stool or notice rectal bleeding
- You have severe or increasing abdominal pain
- You have ongoing nausea or vomiting
These may be signs of bowel obstruction or another serious condition. More laxative is not the answer.
5. Full Side Effect Profile of MiraLax
Expected Effects (These Mean It’s Working)
- Loose, soft, or more frequent stools — this is the intended outcome
Mild Side Effects (Reported by Some Users)
- Mild nausea
- Abdominal bloating or feeling of fullness
- Gas — much less common than with lactulose (because MiraLax is not fermented by gut bacteria)
- Mild abdominal cramping — usually related to taking too much
- Stomach gurgling or rumbling
- Irritation around the anus — from frequent loose stools
Serious Side Effects — Stop Use and Call a Doctor
- Blood in stool or rectal bleeding
- Severe or worsening abdominal pain
- Ongoing diarrhea that is causing dehydration
- Signs of allergic reaction: hives, rash, swelling of the face or throat, difficulty breathing → call 911 immediately
Electrolyte Safety Note
At the normal OTC dose (17 g/day for up to 7 days), MiraLax does not significantly affect electrolytes in healthy adults. However, people with kidney disease, heart failure, or elderly people may be at risk for electrolyte problems with high doses or extended use:
- Low sodium (hyponatremia) — if large amounts draw too much fluid into the colon
- Low potassium (hypokalemia) — from excessive diarrhea at high doses
6. Drug Interactions
MiraLax is not absorbed into your bloodstream, so it has no direct chemical interactions with other drugs. However, because it speeds up how fast things move through your intestines, it can affect how much of other medications your body absorbs.
⚠ Most Important: Starch-Based Thickeners (Listed on Drug Label)
MiraLax reduces the effectiveness of starch-based thickeners that are added to drinks for people who have difficulty swallowing (dysphagia). Affected products include: Thick-It (cornstarch), SimplyThick (xanthan gum), arrowroot starch, tapioca starch, and wheat flour. Always mix MiraLax in a regular, unthickened drink. This is a patient safety issue — incorrect thickener consistency can cause choking in people with swallowing problems.
Warfarin (Coumadin, Jantoven) — Blood Thinner
Faster gut movement can reduce how well warfarin is absorbed. If you take warfarin, tell your doctor before starting MiraLax. Your blood (INR) level may need more frequent monitoring.
Narrow Therapeutic Index Drugs
These are drugs where the gap between an effective dose and a dangerous dose is very small — for example: digoxin (for the heart), certain antibiotics, immunosuppressants. If MiraLax moves these through your system too quickly, less may be absorbed. Ask your pharmacist about any medications like this.
Extended-Release (ER/XR) Pills
ER pills are designed to release medicine slowly over many hours as they travel through your intestines. If MiraLax speeds transit too much, the pill may pass through before it fully dissolves, reducing the drug’s effect. Ask your pharmacist about any ER medications you take.
7. All 6 Types of OTC Laxatives Explained
To understand where MiraLax fits, you need to know all six types of OTC laxatives. Each works differently, has a different onset time, and is best for different situations.
Type 1: Osmotic Laxatives — Draw Water In
How they work: Pull water into the colon to soften stool. They do not stimulate the colon nerves.
Products: MiraLax (PEG 3350), Milk of Magnesia, magnesium citrate, lactulose (prescription in the US)
2023 AGA-ACG Guideline: PEG 3350 — Strong recommendation for chronic use (the only OTC laxative to achieve this). Magnesium oxide — Conditional recommendation. Lactulose — Conditional, only after other OTC options fail.
Time to work: PEG: 1–3 days. Magnesium products: 30 minutes to 6 hours.
Cramping risk: 🟢 Low with PEG. 🟡 Moderate with magnesium. 🔴 High with lactulose (because lactulose is fermented by bacteria, producing gas).
Type 2: Stimulant Laxatives — Force the Colon to Move
How they work: Stimulate the nerve cells (mainly the myenteric/Auerbach’s plexus) in the colon wall, forcing muscle contractions. They also slow fluid absorption from the colon. Bisacodyl is activated by enzymes in the colon lining. Senna is activated by colon bacteria.
Products: Bisacodyl (Dulcolax tablets, Correctol), senna/sennosides (Senokot, Ex-Lax), sodium picosulfate
2023 AGA-ACG Guideline: Bisacodyl/sodium picosulfate — Strong recommendation, but for short-term use (under 4 weeks) or as rescue therapy only. Senna — Conditional recommendation (low certainty evidence).
Time to work: Oral tablets: 6–12 hours. Bisacodyl suppositories: 15–60 minutes.
Cramping risk: 🔴 High — cramping and urgency are common because these drugs force the colon to contract instead of letting it respond naturally.
Long-term use? Not recommended. The 2023 guideline classifies bisacodyl/SPS specifically as short-term or rescue therapy.
You may have heard that long-term stimulant laxatives cause irreversible nerve damage. Current evidence (StatPearls NBK547733) says this risk is rare and it’s unclear whether it comes from the laxatives or from the constipation itself. This concern appears to have been overstated historically. That said, stimulant laxatives are still not meant for daily long-term use.
Type 3: Bulk-Forming Laxatives — Add Fiber to Your Stool
How they work: The fiber soaks up water and physically swells inside the colon, making stool bigger and heavier. This stretching triggers the colon’s natural movement. This is different from osmosis — the fiber physically holds water rather than chemically drawing it in.
Products: Psyllium husk (Metamucil, Konsyl), methylcellulose (Citrucel), wheat dextrin (Benefiber), calcium polycarbophil (FiberCon)
2023 AGA-ACG Guideline: Fiber (psyllium, bran, methylcellulose, inulin) — Conditional recommendation, low certainty evidence.
Time to work: 12–72 hours
Cramping risk: 🟢 Low to moderate. Can cause gas and bloating, especially if you start with too much or don’t drink enough water. Citrucel (methylcellulose) causes less gas than psyllium because it is fermented less by gut bacteria — a good option for people with IBS who get gas from psyllium.
Type 4: Stool Softeners — Make Stool Easier to Pass
How they work: Docusate sodium works like a soap — it breaks the surface tension between water and fat inside the stool, letting water soak in. This makes stool softer. It does not make the colon move — it only softens what is already there.
Products: Colace (docusate sodium 100 mg), Surfak (docusate calcium 240 mg)
Evidence: Multiple systematic reviews found docusate no more effective than placebo for treating constipation. The Choosing Wisely campaign (a major US medical quality initiative) recommends against routine docusate prescribing for constipation. The 2021 Rao & Brenner review found “poor evidence to support its use.” The 2023 AGA-ACG guideline noted docusate for review but issued no recommendation.
Time to work: 24–72 hours (stool softening only, not bowel movement)
Cramping risk: 🟢 Very low
Bottom line: Colace does not reliably cause a bowel movement. It only reduces straining. It is useful after surgery, after childbirth, or for hemorrhoid management — but it is not a treatment for constipation. If you have trouble going to the bathroom, Colace will not fix that. MiraLax is the far better-evidenced choice.
Type 5: Lubricant Laxatives — Oil the Passage
How they work: Mineral oil coats the stool and the intestinal lining with a waterproof film, making stool slippery and easier to pass.
Products: Mineral oil (oral liquid; Fleet Mineral Oil Enema)
Time to work: 6–8 hours orally
Important warnings:
- Never take lying down — oil can accidentally enter the lungs (lipoid pneumonia)
- Take at least 2 hours away from meals — blocks absorption of vitamins A, D, E, and K
- Not safe for elderly people or anyone with difficulty swallowing
- Not recommended for long-term use
Type 6: Enemas and Suppositories — Act Directly in the Rectum
How they work: Inserted directly into the rectum. They work locally on the lower colon only — not the upper colon where most constipation originates.
Products: Glycerin suppositories, bisacodyl suppositories (Dulcolax suppository), Fleet Enema (sodium phosphate), mineral oil enema
Time to work: Glycerin: 15–30 minutes. Bisacodyl suppository: 15–60 minutes.
Cramping risk: 🟢 Low for glycerin. 🟡 Mild to moderate for bisacodyl suppository.
Key point vs. MiraLax: These work only on the last part of the colon (the rectum and sigmoid). MiraLax works throughout the entire colon — it is more effective for constipation that originates higher up.
Best use: When stool is stuck in the rectum (impaction), when oral laxatives have not worked, or when you need very fast relief.
8. MiraLax vs. Every Major OTC Laxative: Master Comparison Table
| Product | Type | Time to Work | Cramping Risk | 2023 Guideline Grade | Safe Long-Term? | Best Use Case |
|---|---|---|---|---|---|---|
| MiraLax (PEG 3350) | Osmotic | 1–3 days | 🟢 Low | Strong — the only OTC laxative with strong rec. for chronic use | ✅ Yes, under doctor supervision | Chronic constipation; opioid-induced constipation; daily ongoing management |
| Milk of Magnesia | Osmotic (saline) | 30 min–6 hrs | 🟡 Moderate | Conditional (magnesium oxide reviewed) | ⚠️ No — electrolyte risk | Quick one-time relief when speed matters |
| Magnesium Citrate | Osmotic (saline) | 30 min–6 hrs | 🟡 Moderate | Not reviewed in 2023 guideline | ⚠️ No — electrolyte risk | Acute one-time relief; partial colonoscopy prep |
| Lactulose (Rx-only in US) | Osmotic (via bacterial fermentation) | 24–48 hrs | 🔴 High (gas & bloating) | Conditional — only after other OTC options fail; very low certainty | ✅ Yes, for hepatic encephalopathy | Liver disease (hepatic encephalopathy); constipation second-line only |
| Dulcolax tablets (bisacodyl) | Stimulant | 6–12 hrs | 🔴 High | Strong — but short-term (<4 weeks) or rescue use only | ⚠️ No — short-term/rescue only per guideline | Fast relief when speed matters; rescue therapy; pre-procedure prep |
| Dulcolax suppository | Stimulant (rectal) | 15–60 min | 🟡 Moderate | Included in bisacodyl strong rec. (short-term) | ⚠️ No — short-term rectal use only | Fastest relief; rectal impaction; pre-procedure |
| Senokot / Ex-Lax (senna) | Stimulant | 6–12 hrs | 🔴 High | Conditional (low certainty evidence)† | ⚠️ Caution — long-term data limited | Acute relief; rescue use alongside MiraLax |
| Metamucil (psyllium) | Bulk-forming fiber | 12–72 hrs | 🟢 Low (gas possible) | Conditional (low certainty evidence) | ✅ Yes — also supports gut health | Mild constipation; lowering cholesterol; long-term gut health |
| Citrucel (methylcellulose) | Bulk-forming fiber | 12–72 hrs | 🟢 Low (less gas than psyllium) | Included in fiber conditional rec. | ✅ Yes | Mild constipation; IBS patients who get too much gas from psyllium |
| Colace (docusate sodium) | Stool softener | 24–72 hrs | 🟢 Very low | No recommendation — evidence no better than placebo for constipation | ⚠️ Short-term only; does not treat constipation | Preventing straining after surgery or childbirth; hemorrhoids — NOT constipation treatment |
| Mineral Oil | Lubricant | 6–8 hrs | 🟢 Low | Insufficient evidence | ⚠️ No — blocks vitamin absorption long-term | Short-term only; avoid in elderly or people with swallowing difficulty |
| Glycerin Suppository | Rectal (osmotic/lubricant) | 15–30 min | 🟢 Very low | Not reviewed in 2023 guideline | ⚠️ Rectal use only; not for daily management | Fast local rectal relief; gentle and safe in elderly patients |
| Fleet Enema (sodium phosphate) | Rectal (saline) | 1–5 min | 🟡 Moderate | Not reviewed; kidney and electrolyte risk | ⚠️ No — serious electrolyte risk | Acute rectal impaction; pre-procedure prep only |
†Senna note: The 2021 Rao & Brenner review (funded by Bayer US LLC) gave senna a Grade A rating. The 2023 AGA-ACG guideline (independently funded by AGA and ACG) downgraded senna to a conditional recommendation with low certainty of evidence. PEG 3350 received a strong recommendation in both frameworks — the only OTC laxative to do so.
9. MiraLax vs. Lactulose: Deep Dive
Both MiraLax and lactulose are called “osmotic laxatives,” but they work in very different ways. Understanding this difference explains their very different side effect profiles.
How MiraLax Works vs. How Lactulose Works
MiraLax (PEG 3350):
- Physically bonds with water molecules and holds them in the stool
- Gut bacteria cannot break it down → no gas is produced
- The effect is entirely physical (osmosis) — no chemistry, no fermentation
- Result: soft stool, no bloating, no gas
Lactulose:
- A synthetic sugar that human enzymes cannot digest
- Gut bacteria ferment it in the colon → producing lactic acid, acetic acid, and gases: hydrogen (H₂), methane (CH₄), carbon dioxide (CO₂)
- These gases are why lactulose commonly causes bloating, flatulence, and cramping
- The osmotic drawing of water is a secondary effect that comes after fermentation
Side-by-Side Comparison
| Feature | MiraLax (PEG 3350) | Lactulose (Enulose, Generlac, Kristalose) |
|---|---|---|
| Prescription needed in US? | No — buy OTC at any pharmacy | Yes — requires a doctor’s prescription in the US (available OTC in Bangladesh, UK, India, and many other countries) |
| FDA approval history | Prescription: 1999. OTC: 2006. | Prescription only since 1977 |
| How fast does it work? | 1–3 days | 24–48 hours |
| Gas and bloating? | 🟢 Low — no fermentation, no gas | 🔴 High — fermentation produces H₂, CH₄, and CO₂ |
| Cramping? | 🟢 Unlikely at correct dose | 🔴 Common — listed as a common side effect on its FDA label |
| Taste and form | Tasteless powder — mixes invisibly into any drink | Sweet syrup or crystals — many patients find it unpleasant |
| Safe for people with diabetes? | ✅ Yes — contains no sugar, no effect on blood glucose | ⚠️ Use caution — the syrup form contains galactose and lactose |
| Effect on gut bacteria (microbiome)? | None — not fermented, does not alter gut bacteria | ✅ Prebiotic effect — promotes beneficial bacteria (Lactobacilli, Bifidobacteria) |
| Treats liver disease (hepatic encephalopathy)? | ❌ No — cannot reduce ammonia levels | ✅ Yes — gold standard treatment for this condition |
| 2023 AGA-ACG guideline recommendation | Strong recommendation for chronic use | Conditional — only after OTC options have failed; very low certainty evidence |
What Does the Research Actually Show?
The 2010 Cochrane systematic review (Lee-Robichaud et al., CD007570) compared PEG directly against lactulose across multiple randomized controlled trials. PEG was found to be better on:
- Number of bowel movements per week
- Stool consistency
- Abdominal pain relief
- Need for additional laxatives
The 2023 AGA-ACG guideline strongly recommends PEG for chronic constipation and only suggests lactulose as a fallback for patients who cannot tolerate or do not respond to standard OTC therapies — with very low certainty of evidence. This is a significant step down from lactulose’s older reputation.
When Is Lactulose the Better Choice?
Lactulose is essential for hepatic encephalopathy — a brain complication of liver disease where ammonia builds up in the blood. Here is how it works:
- The fermentation acids lower the pH (make the colon more acidic)
- This converts absorbable ammonia (NH₃) into non-absorbable ammonium (NH₄⁺)
- The ammonium gets trapped in the stool and excreted from the body
👉 MiraLax has no effect on ammonia and cannot replace lactulose in this condition.
10. MiraLax Dosage Guide (Adults + Children)
Standard Adult Dose (Ages 17 and Older)
| What | Details |
|---|---|
| Amount | 17 grams — fill the capful to the white line inside the cap, or use one pre-measured single-dose packet |
| How often | Once per day |
| How to mix | Stir into 4–8 oz (120–240 mL) of any beverage — water, juice, coffee, tea, soda (hot or cold). Make sure the powder is fully dissolved before drinking. No clumps. |
| When to take | Any time of day, with or without food. Consistent timing (same time each day) can help you get consistent results. |
| Do NOT mix with | Starch-based drink thickeners (cornstarch, xanthan gum, arrowroot, tapioca starch) — MiraLax breaks down these thickeners, which is dangerous for people with swallowing difficulties |
| When it starts working | Usually a bowel movement in 1–3 days. Best results often seen after a week of consistent daily use. |
| Maximum OTC use | 7 days without a doctor’s supervision |
What to Do If You Miss a Dose
Take it as soon as you remember. If it is almost time for your next dose, skip the missed one. Do not take two doses to make up for a missed one — this causes diarrhea and cramping.
Signs You Are Taking Too Much
- Watery, runny diarrhea
- Sudden urgent need to go to the bathroom
- Abdominal cramping
If these happen: reduce your dose or stop, and speak with a pharmacist or doctor.
Children’s Dosing — Always Requires a Doctor’s Approval
MiraLax is not FDA-approved for OTC use in children under 17. However, it is among the most commonly prescribed constipation treatments in children, per NASPGHAN and ESPGHAN guidelines (Tabbers et al., J Pediatr Gastroenterol Nutr, 2014). A doctor will calculate the dose based on the child’s weight:
| Child’s Age | Typical Doctor-Prescribed Dose |
|---|---|
| 6 months – 2 years | Individualized by doctor (0.5–1.5 g/kg/day) |
| 2–11 years | 0.4–0.8 g/kg/day (often 8.5–17 g/day); adjusted for 1–2 soft stools/day |
| 12–16 years | Close to adult dose (~17 g/day); still needs doctor supervision |
The FDA has received reports of behavioral changes in some children taking PEG 3350 — including tics, obsessive-compulsive behavior, and anxiety. A large safety study was commissioned. As of now, a definitive cause-and-effect link has not been established in controlled clinical trials. However, parents and doctors should be aware of this concern and report any worrying behavioral changes promptly.Never give MiraLax to a child without first consulting a pediatrician or pediatric gastroenterologist.
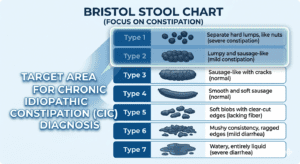
11. Bristol Stool Scale: Is MiraLax Working for You?
Clinical trials that test MiraLax use the Bristol Stool Form Scale (BSFS) to measure whether it is working. The scale was validated by Lewis & Heaton (1997) and is used worldwide by doctors. Here is how to read your own results:
| Type | What It Looks Like | What It Means for MiraLax Users |
|---|---|---|
| Type 1 | Separate hard lumps — like small pellets or nuts | Severe constipation. MiraLax needs more time. If no improvement after 3 days, see a doctor. |
| Type 2 | Lumpy sausage shape — hard and lumpy | Mild constipation. Give MiraLax more time and drink more water. |
| Type 3 | Sausage shape with cracks on the surface | ✅ Ideal result — MiraLax is working correctly. |
| Type 4 | Smooth, soft sausage or snake shape | ✅ Ideal result — MiraLax is working correctly. |
| Type 5 | Soft blobs with clear-cut edges | Slightly loose — consider reducing your dose a little. |
| Type 6 | Mushy, fluffy pieces — no defined shape | Dose is too high. Reduce your MiraLax dose. |
| Type 7 | Entirely liquid — completely watery | Stop MiraLax. Rehydrate with water or an electrolyte drink (Gatorade, Pedialyte). |
👉 Target: Type 3 or Type 4 consistently
👉 Getting Type 6 or 7 regularly? → Reduce your dose
👉 Still Type 1 or 2 after 3+ days? → Talk to a doctor before increasing dose
12. How Long Can You Take MiraLax?
The OTC label says: no more than 7 days without a doctor’s supervision. The reason is that ongoing constipation usually has an underlying cause — a poor diet, a medication side effect, a thyroid problem, or a bowel motility disorder — that should be found and treated, not just masked with a laxative indefinitely.
Long-Term Use: Only Under a Doctor’s Supervision
The 2023 AGA-ACG guideline gave PEG the only strong recommendation for long-term (chronic) use among all OTC laxatives. Doctors can prescribe it long-term for:
- Chronic idiopathic constipation (CIC) — studied safely for up to 6 months
- Opioid-induced constipation — used alongside ongoing opioid therapy
- Slow-transit constipation — as part of a broader treatment plan
- Children with functional constipation — off-label use per NASPGHAN/ESPGHAN guidelines, often for several months
With long-term use, doctors use the lowest effective dose and periodically check electrolyte levels, especially in elderly patients or those with kidney problems.
Is MiraLax Habit-Forming?
The label says PEG 3350 “may be habit-forming.” But NASPGHAN’s clinical FAQ explains this clearly:
“PEG 3350 works by keeping more water in the stool so it is softer and easier to pass. It does not work on the nerves or muscles of the gut and so does not cause any dependence or damage.”— NASPGHAN PEG 3350 Expert FAQ
The label warning is a standard regulatory phrase required for all laxatives — not a reflection of true physiological addiction with PEG specifically. Best practice: use MiraLax for relief while also improving fiber, water intake, and physical activity to tackle the root cause.
13. MiraLax for Colonoscopy Prep
MiraLax is also used at much higher doses to completely empty the colon before a colonoscopy — a procedure to check the inside of the colon for polyps or cancer.
Standard Low-Volume MiraLax Prep Protocol
- 238 grams of MiraLax (about 14 standard doses) dissolved completely in 64 oz of Gatorade or Powerade
- Given as a split dose: drink half the evening before the procedure, drink the other half the morning of the procedure
- Follow a clear liquid diet the full day before
- Finish the morning portion at least 2 hours before your arrival time
At colonoscopy-prep doses, MiraLax draws huge amounts of water into the colon. Plain water would cause dangerous electrolyte losses — especially risky for elderly patients or those with kidney or heart disease. Gatorade contains electrolytes (sodium, potassium) that help replace what is lost.Important: Always follow your gastroenterologist’s exact protocol. Do not substitute without their approval. Commercial prep kits (GoLYTELY, MoviPrep, NuLYTELY) contain different formulations and are not the same thing as mixing standard OTC MiraLax powder with Gatorade.
14. Overdose and Accidental Ingestion
MiraLax has low toxicity, but taking significantly more than 17 g/day — accidentally or intentionally — can cause serious problems.
Signs of Too Much MiraLax
- Severe, watery, or explosive diarrhea
- Intense abdominal cramping
- Nausea and vomiting
- Signs of dehydration: dry mouth, dizziness, rapid heartbeat, very little urination, dark urine
- Electrolyte problems: muscle weakness, confusion, irregular heartbeat, extreme fatigue
What To Do — Step by Step
- 🛑 Stop taking MiraLax immediately
- 📞 Call Poison Control (US): 1-800-222-1222 — available 24/7. Tell them the person’s weight and approximately how much was taken.
- 💧 Start rehydrating — water or an electrolyte drink (Pedialyte, Gatorade)
- 🚨 Go to the emergency room immediately if you notice: severe confusion, inability to keep any fluids down, extreme dizziness, very little or no urination, chest pain, or fast or irregular heartbeat
Call 1-800-222-1222 right away. PEG 3350 is not acutely toxic, but a small child can become dangerously dehydrated quickly from the resulting diarrhea. Have the child’s weight and estimated amount ingested ready when you call.
15. Storage Instructions
- 🌡️ Temperature: Store at room temperature — 59–77°F (15–25°C). Do not leave in a hot car, near a stove, or in direct sunlight.
- 💧 Moisture: Keep the cap tightly closed at all times. Avoid storing in the bathroom medicine cabinet (too humid). A bedroom drawer or kitchen cabinet away from the sink is better.
- 👶 Children and pets: Store out of reach. The tasteless powder looks harmless and can easily be accidentally eaten.
- 📅 Expiration date: Do not use past the printed expiration date. Over time, PEG 3350 absorbs moisture and may clump, preventing it from fully dissolving.
- 🥤 Pre-mixed solution: If you mix MiraLax in advance (for travel or convenience), refrigerate the solution and use it within 24 hours.
16. Who Should Avoid MiraLax?
Do NOT Use MiraLax If You Have:
- Known allergy to polyethylene glycol — rare but it happens. Stop immediately if you develop hives, rash, or swelling. Call 911 if you have any trouble breathing.
- Known or suspected bowel obstruction — do not take any laxative. Go to the doctor right away.
Talk to Your Doctor First If You Have:
- Kidney disease — the OTC label requires physician consultation. Your kidneys may be less able to manage the fluid shifts caused by MiraLax.
- Heart failure or need to restrict fluids — talk to your cardiologist before using MiraLax.
- Nausea, vomiting, or severe abdominal pain — these can be signs of a bowel obstruction. Do not take laxatives.
- A change in bowel habits lasting more than 2 weeks — this needs medical evaluation to rule out colorectal cancer or inflammatory bowel disease (Crohn’s, ulcerative colitis).
- IBS (irritable bowel syndrome) — your gut is more sensitive. Evidence is stronger for CIC than IBS-C. A doctor can advise on appropriate use.
- Difficulty swallowing (dysphagia) — especially if you use starch-based thickeners in your drinks. See the Drug Interactions section.
Special Situations
- Pregnant or breastfeeding: MiraLax is not absorbed into the bloodstream, which is reassuring. Many OB-GYNs recommend it when dietary changes are not enough. The label says: “If pregnant or breast-feeding, ask a health professional before use.” Always follow this advice.
- Children under 17: Not approved for OTC use in this group. Doctor supervision and weight-based dosing are required. See pediatric dosing section above.
- Elderly patients: Generally well-tolerated in clinical trials. However, elderly people are more likely to become dehydrated, so adequate fluid intake is especially important. Electrolyte monitoring is wise with extended use.
- Taking prescription medications: Always tell your pharmacist you are taking MiraLax. See the Drug Interactions section for which medications to be most careful with.
17. When MiraLax Doesn’t Work: Next Steps
After 3 Days With No Bowel Movement — Try These First
- ✅ Double-check you’re using exactly 17 g and that it is fully dissolved in at least 4 oz of liquid
- ✅ Increase your water intake to 8–10 glasses (64–80 oz) per day
- ✅ Take MiraLax at least 2 hours away from other medications
- ✅ Add dietary fiber to your diet — prunes, psyllium husk, or kiwifruit alongside MiraLax
- ✅ Try taking it at a different time of day (some people respond better in the morning, others at night)
- ✅ Walk for at least 20–30 minutes — physical activity stimulates the bowel
After 7 Days With Inadequate Relief — See a Doctor
Your doctor may adjust the dose of MiraLax, add a short-term stimulant laxative (bisacodyl as rescue therapy, per the 2023 guideline), or refer you for testing.
Prescription Options When OTC Laxatives Fail
| Medication | Brand | How It Works (Simple) | 2023 AGA-ACG Status |
|---|---|---|---|
| Linaclotide | Linzess | Signals the intestine to release more fluid and move faster | Strong rec. — after OTC failure |
| Plecanatide | Trulance | Same family as linaclotide — similar mechanism | Strong rec. — after OTC failure |
| Prucalopride | Motegrity | Directly activates receptors to make the colon move faster | Strong rec. — after OTC failure |
| Lubiprostone | Amitiza | Opens chloride channels, pulling fluid into the intestine | Conditional rec. — after OTC failure |
| Methylnaltrexone | Relistor | Blocks the gut effects of opioids without affecting pain relief | For opioid-induced constipation only |
| Naloxegol | Movantik | Same — blocks opioid effects in the gut | For opioid-induced constipation only |
Tests Your Doctor May Order
- Colonoscopy — rules out structural problems like polyps, strictures, or colorectal cancer
- Colonic transit study — measures how fast stool moves through your colon (uses small markers or a swallowed capsule)
- Anorectal manometry — checks your pelvic floor muscles; dyssynergic defecation (a coordination problem between pushing and relaxing) is a very common and very treatable cause of constipation
- MRI defecography — shows what happens structurally during defecation
- Blood tests — TSH (thyroid), calcium, and blood glucose to check for hypothyroidism, hypercalcemia, or diabetes as contributing causes
📖 See also:
18. Product Recommendations
🛒 MiraLax Original — Standard 30-Dose Bottle
The brand-name product. Tasteless, grit-free — mixes completely in any beverage. Available at every US pharmacy and online.
🛒 MiraLax 45-Dose Bottle — Best Value
Larger bottle for long-term use under physician supervision. Same formula, lower cost per dose.
🛒 MiraLax Single-Use Packets (24 Count) — Travel Friendly
Pre-measured 17 g packets — no measuring, no mess. Perfect for travel, work, or keeping in your bag. Each packet delivers exactly the correct dose.
🛒 Amazon Basic Care ClearLax — Generic PEG 3350 (Best Price)
Therapeutically identical to MiraLax — same active ingredient (PEG 3350) at the same 17 g dose. The FDA has confirmed no meaningful difference between brand and generic PEG 3350. A smart, economical choice.
🌿 Natural Osmotic Alternative: NOW Foods Magnesium Citrate Powder (iHerb)
Prefer a more natural option? Magnesium citrate draws water into the colon through osmosis — similar to MiraLax but acting faster (within hours, not days). Better suited for occasional use than daily management. The 2023 AGA-ACG guideline gave magnesium oxide a conditional recommendation.
19. Natural Alternatives to MiraLax
Prefer to avoid OTC laxatives, or want to use MiraLax only occasionally while building lasting gut health? These evidence-backed approaches are worth trying:
- 🌾 Psyllium husk (Metamucil) — bulk-forming fiber; conditional recommendation (2023 AGA-ACG); takes 1–3 days; also lowers LDL cholesterol. Must be taken with plenty of water. See: Natural Constipation Relief Protocol.
- 🧲 Magnesium citrate or oxide — osmotic agents that draw water into the colon. Magnesium oxide received a conditional recommendation in the 2023 AGA-ACG guideline. Acts faster than MiraLax. See: Best Magnesium for Constipation.
- 🫒 Extra-virgin olive oil — lubricates the intestinal lining and stimulates the colon via polyphenols. Clinical studies support its use for constipation relief. See: Olive Oil for Constipation.
- 🍇 Prunes and prune juice — contain sorbitol (a natural osmotic laxative) plus phenolic compounds that stimulate the colon. Backed by multiple randomized controlled trials.
- 🥝 Kiwifruit — 2 kiwis per day shown to improve constipation in clinical studies; included in Rao & Brenner 2021 as part of the fruit-based laxative category (Grade B).
- 🌰 Castor oil pack — topical approach placed on the abdomen; some evidence for stimulating intestinal movement via ricinoleic acid. See: How to Use a Castor Oil Pack.
- 🦠 Probiotics — specific strains (Bifidobacterium spp., Lactobacillus spp.) can improve stool frequency and consistency by supporting a healthy gut microbiome.
- 💧 Water + fiber + movement — the foundation — Aim for 8–10 glasses of water daily, 25–35 grams of dietary fiber from whole foods, and 30+ minutes of moderate exercise most days. The majority of occasional constipation cases improve with these changes alone.
📖 See also: 5 Steps to Natural Constipation Relief Protocol
20. Frequently Asked Questions
Does MiraLax cause cramping?
At the standard dose of 17 g/day, MiraLax does not typically cause cramping. It works by holding water in the stool through osmosis — not by stimulating colon nerves. Multiple clinical trials confirm this. Cramping can occur if you take too much, have IBS-C, are dehydrated, or have an underlying GI condition. If cramping gets worse while using MiraLax, stop and see a doctor.
How does MiraLax compare to Dulcolax?
They are fundamentally different types. MiraLax = osmotic. Dulcolax (bisacodyl) = stimulant. Dulcolax works in 6–12 hours by forcing nerve-driven colon contractions — which commonly causes cramping and urgency. MiraLax takes 1–3 days but is much gentler. The 2023 AGA-ACG guideline recommends MiraLax for chronic daily use and Dulcolax only for short-term or rescue use (under 4 weeks). Both have valid roles — just in different situations.
Is Colace (docusate) the same as MiraLax?
No — they are not the same and cannot be substituted. Colace softens stool to reduce straining but does not reliably produce bowel movements. Multiple systematic reviews found it no more effective than placebo for treating constipation. MiraLax has strong evidence and a strong guideline recommendation. Colace is useful for preventing straining after surgery, childbirth, or with hemorrhoids — but it does not treat constipation itself.
How does MiraLax compare to Metamucil (psyllium fiber)?
Both take 1–3 days but work differently. Metamucil adds physical fiber bulk to stimulate movement; MiraLax draws water osmotically to soften stool. The 2023 AGA-ACG guideline gives PEG a strong recommendation and psyllium only a conditional one. Metamucil also lowers cholesterol and feeds beneficial gut bacteria — benefits MiraLax does not provide. For mild constipation, fiber is often the right first step. For more serious constipation, medication-induced constipation, or when fiber hasn’t worked, MiraLax is the stronger option.
How long does MiraLax take to work?
Usually 1 to 3 days for the first bowel movement. If you need same-day relief, magnesium citrate or a glycerin suppository are faster alternatives for one-time use.
How long can you safely take MiraLax?
7 days maximum OTC without a doctor’s supervision. Under a doctor’s guidance, long-term use is safe and well-supported — PEG is the only OTC laxative with a strong chronic-use recommendation in the 2023 AGA-ACG guideline. Always get persistent constipation evaluated medically.
Is MiraLax better than Lactulose for constipation?
For standard constipation: yes. The 2010 Cochrane review found PEG better on stool frequency, stool form, pain relief, and need for extra laxatives. The 2023 AGA-ACG guideline strongly recommends PEG and places lactulose only as a fallback when other OTC options fail. For liver disease with high ammonia (hepatic encephalopathy), lactulose remains indispensable — MiraLax cannot replace it.
Can you take MiraLax if you have kidney disease?
Not without a doctor’s approval. The OTC label requires physician consultation for kidney disease patients. Your doctor can advise on whether MiraLax is appropriate, what dose to use, and whether electrolyte monitoring is needed.
Can MiraLax be taken during pregnancy?
MiraLax is not absorbed into the bloodstream, which is reassuring during pregnancy. Many OB-GYNs recommend it when dietary changes aren’t enough. The label says: “If pregnant or breast-feeding, ask a health professional before use.” Always follow this guidance.
Why is MiraLax gentler than senna or bisacodyl?
Senna and bisacodyl directly activate nerve cells in the colon wall, forcing muscle contractions. This produces cramping, urgency, and sudden bowel movements. MiraLax only holds water in the stool — it never touches or stimulates any nerves. The colon responds to the softer, bulkier stool through its own natural rhythm. No forced contractions = no cramping.
Does MiraLax interact with other medications?
Indirectly — yes. MiraLax speeds up gut transit, which can reduce how much of other oral medications your body absorbs, especially warfarin, digoxin, and extended-release pills. Take other medications at least 2 hours before or after MiraLax. Always tell your pharmacist you are taking MiraLax when you pick up a new prescription.
What should I do if I accidentally take too much MiraLax?
Stop immediately and call Poison Control at 1-800-222-1222 (US, available 24/7). Rehydrate with water or an electrolyte drink. Go to the emergency room if you have severe confusion, cannot keep fluids down, extreme dizziness, very little urination, or heart palpitations.
21. References
- Bharucha AE, Wald A. “Chronic Constipation.” Mayo Clin Proc. 2019;94(11):2340–2357. doi:10.1016/j.mayocp.2019.01.031
- Chang L, Chey WD, Imdad A, et al. “American Gastroenterological Association–American College of Gastroenterology Clinical Practice Guideline: Pharmacological Management of Chronic Idiopathic Constipation.” Gastroenterology. 2023;164(7):1086–1106. doi:10.1053/j.gastro.2023.03.214 [Primary source for all evidence grades used in this article — 2023 AGA-ACG Joint Guideline, independently funded by AGA and ACG]
- Rao SSC, Brenner DM. “Efficacy and Safety of Over-the-Counter Therapies for Chronic Constipation: An Updated Systematic Review.” Am J Gastroenterol. 2021;116(6):1156–1181. doi:10.14309/ajg.0000000000001222 [Note: Medical writing support for this review was funded by Bayer US LLC — the manufacturer of MiraLax. PEG’s strong recommendation status was confirmed independently by the 2023 AGA-ACG guideline.]
- Lee-Robichaud H, Thomas K, Morgan J, Nelson RL. “Lactulose versus polyethylene glycol for chronic constipation.” Cochrane Database Syst Rev. 2010;(7):CD007570. doi:10.1002/14651858.CD007570.pub2
- DiPalma JA, Cleveland MvB, McGowan J, Herrera JL. “A randomized, multicenter, placebo-controlled trial of polyethylene glycol laxative for chronic treatment of chronic constipation.” Am J Gastroenterol. 2007;102:1436–1441. doi:10.1111/j.1572-0241.2007.01199.x
- Zurad EG, Johanson JF. “Over-the-counter laxative polyethylene glycol 3350: an evidence-based appraisal.” Curr Med Res Opin. 2011;27(7):1439–1452. doi:10.1185/03007995.2011.580339. PMID:21604961 [Funded by Bayer US LLC]
- Joo JS, Ehrenpreis ED, Gonzalez L, et al. “Polyethylene glycol 3350 in occasional constipation.” World J Gastroenterol. 2016;22(18):4642–4652. PMC:PMC4848251
- Hammer HF. “Polyethylene Glycol.” StatPearls [Internet]. StatPearls Publishing; 2023. NBK557652
- Mukherjee S, Patel P, John S. “Lactulose.” StatPearls [Internet]. StatPearls Publishing; 2024. NBK536930
- Corsetti M, et al. “Bisacodyl: A review of pharmacology and clinical evidence.” Neurogastroenterol Motil. 2021;33(10):e14123. doi:10.1111/nmo.14123
- Sizar O, et al. “Bisacodyl.” StatPearls [Internet]. StatPearls Publishing; 2024. NBK547733
- Tabbers MM, DiLorenzo C, Berger MY, et al. “Evaluation and treatment of functional constipation in infants and children: evidence-based recommendations from ESPGHAN and NASPGHAN.” J Pediatr Gastroenterol Nutr. 2014;58(2):258–274. doi:View MiraLax 30-Dose on Amazon →
- Lewis SJ, Heaton KW. “Stool form scale as a useful guide to intestinal transit time.” Scand J Gastroenterol. 1997;32(9):920–924. doi:10.3109/00365529709011203 [Original validation study for the Bristol Stool Form Scale]
- NASPGHAN. “Polyethylene Glycol 3350 (PEG 3350) Frequently Asked Questions.” GIKids.org. gikids.org
- Chogle A. “Science, concerns behind the MiraLAX laxative debate.” Healio Pediatrics. 2017. healio.com [FDA neuropsychiatric adverse event reports in children — background]
- U.S. National Library of Medicine. “Polyethylene glycol 3350.” MedlinePlus. medlineplus.gov
- U.S. National Library of Medicine. “Lactulose.” MedlinePlus. medlineplus.gov
- Bayer Consumer Health. “About MiraLAX.” miralax.com
- U.S. FDA. “Drug Approval Package: MiraLax NDA# 20-698.” February 18, 1999. FDA.gov
- Federal Register. “Opportunity for Hearing on a Proposal to Withdraw Approval of Prescription PEG 3350 ANDAs.” October 24, 2008. federalregister.gov [Confirms OTC approval October 6, 2006]
- American Association of Poison Control Centers. Poison Help: 1-800-222-1222. poisonhelp.org
📚 Related Articles on Constipation Relief:
- Best OTC Laxatives for Constipation in the US — Full Buyer’s Guide
- Best Magnesium for Constipation: Oxide vs. Citrate vs. Glycinate
- Olive Oil for Constipation — Clinical Evidence Review
- How to Use a Castor Oil Pack for Constipation
- Mag O7 vs Oxy-Powder: Which Is Best?
- 5 Steps to Natural Constipation Relief Protocol
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Consult with a licensed healthcare professional before starting any supplement regimen, especially if you are pregnant, nursing, have kidney disease, or take prescription medications. Individual results may vary. The experiences shared by community members are their own and do not constitute medical claims.
Affiliate Disclosure: This page contains affiliate links to Amazon and iHerb. We may earn a commission at no extra cost to you. Our recommendations are independent and based on research and community feedback.










[…] MiraLax (PEG 3350) — An osmotic laxative. A tasteless powder mixed into any drink. It travels through the gut retaining water in the stool, keeping it soft until it passes naturally. Generally considered the gentlest option of the three. See our guide on MiraLax side effects and cramping causes […]