Sitting on the toilet but feeling like your poop stuck but won’t come out can be uncomfortable, frustrating, and stressful. Many adults experience this problem at some point in their lives. You may spend minutes—or even hours—trying to pass stool, only to feel incomplete relief. This can cause bloating, abdominal pressure, and constant discomfort.
In medical terms, this situation is often related to severe constipation or Fecal Impaction. This occurs when stool stays in the large intestine for too long, becomes dry and hard, and cannot pass naturally.
Why Constipation Happens
Constipation often develops due to low fiber intake, dehydration, lack of physical activity, or certain medications. Studies suggest that nearly 12–19% of adults worldwide experience chronic constipation. Experts from Mayo Clinic and National Institute of Diabetes and Digestive and Kidney Diseases warn that untreated chronic constipation can lead to complications such as hemorrhoids, anal fissures, or other anorectal problems.
The good news is that with the right diet, lifestyle habits, and safe medical strategies, most people can relieve constipation naturally and prevent it in the future.
What You’ll Learn in This Guide
This ultimate guide will provide science-backed solutions to help you relieve constipation quickly and safely. By reading this guide, you will learn:
-
Why poop gets stuck and the science behind fecal impaction
-
How severe constipation differs from occasional constipation
-
Immediate steps to take when stool won’t pass
-
The correct toilet posture that makes bowel movements easier
-
Foods, habits, and diets that naturally improve digestion
-
Safe laxatives and natural remedies, including proper dosages and side effects
-
Special advice for children, pregnant women, and older adults
-
Possible complications of long-term constipation and warning signs
-
When to see a doctor for constipation
-
Lifestyle changes that prevent constipation in the long term
By following this guide, you can achieve fast relief from stuck stool while supporting your overall gut health and digestive wellness.
Immediate Relief Options: What to Use When Poop is Stuck but Won’t Come Out
| Type of Remedy | Examples | Action Speed | Best Used For | Shop Link |
| Bulk-Forming | FiberCon Fiber Therapy Caplets | 12–72 Hours | People who want relief without gas or bloating. | Check |
| Osmotic Laxative | Polyethylene Glycol, Magnesium | 6–48 Hours | Gentle relief for chronic constipation. | Check |
| Stimulant | Senna, Bisacodyl | 6–12 Hours | Emergency “overnight” relief only. | Check |
| Stool Softener | Docusate Sodium | 12–72 Hours | Easier passage after surgery or pain. | Check |
| Synbiotics | Probiotics + Prebiotic Fiber | Long-term | Restoring gut health and internal rhythm. | Check |
| Immediate Aid | Glycerin Suppositories | 15–30 Mins | When stool is physically stuck at the exit. | Check |
Why Your Poop Stuck But Won’t Come Out: Common Causes
The sensation that stool is lodged in the rectum and cannot be expelled is more than just an inconvenience; it is often the precursor to a serious condition known as Fecal Impaction. Understanding the physiological mechanisms behind this “stuck” feeling is essential for finding long-term relief.
Colonic Transit and the Role of Dehydration
The primary function of the colon (large intestine) is to absorb water and electrolytes from digested food. Under normal circumstances, stool moves through the colon within 12 to 48 hours.
-
The Mechanism of Hard Stool: According to the Mayo Clinic, when bowel motility slows down, the colon absorbs excessive amounts of water from the waste. This results in stool that is dry, dense, and stone-like.
-
The “Stuck” Sensation: Dry stool creates significant friction against the intestinal walls. Without sufficient lubrication, natural peristalsis (the wave-like muscle contractions) is unable to push the mass forward, leading to the feeling of being “stuck.”
Muscle Coordination and Pelvic Floor Dyssynergia
Defecation is a highly coordinated neuromuscular event. A key player in this process is the Puborectalis muscle, which wraps around the rectum like a sling to maintain the anorectal angle.
-
Normal Function: During a bowel movement, the brain signals the puborectalis and external anal sphincter to relax, straightening the rectum and allowing stool to pass.
-
Pelvic Floor Dyssynergia: Research published by Harvard Health suggests that in some individuals, these muscles fail to relax or may even contract paradoxically during straining. This condition, known as Pelvic Floor Dyssynergia, makes it feel as though the exit is “blocked,” even if the stool itself is not exceptionally hard. Chronic straining from this condition often leads to complications like hemorrhoids and anal fissures.
Medical Conditions Affecting Gut Motility
Intestinal movement is governed by the autonomic nervous system and endocrine signals. Several clinical conditions can significantly disrupt this “Gut Motility”:
-
Irritable Bowel Syndrome (IBS): As noted by the NIDDK, IBS can cause irregular muscle contractions in the colon, leading to bouts of severe constipation (IBS-C).
-
Diabetes and Neuropathy: Long-term hyperglycemia can damage the nerves controlling the digestive tract (Autonomic Neuropathy), leading to a sluggish bowel.
-
Hypothyroidism: According to the American Thyroid Association, an underactive thyroid slows down the body’s entire metabolism, which directly impacts the speed of intestinal contractions.
Medication-Induced Constipation
Many common pharmaceutical interventions have a profound impact on bowel regularity. The Cleveland Clinic identifies several classes of drugs that contribute to fecal impaction:
-
Opioids: Pain medications frequently bind to receptors in the gut, effectively “freezing” the digestive process.
-
Iron Supplements: These often increase the density of the stool, making it darker, harder, and more difficult to pass.
-
Antidepressants: Certain psychiatric medications can interfere with the chemical signals required for smooth muscle relaxation in the intestines.
How Severe Constipation Differs from Occasional Constipation
Not all constipation is created equal. While almost everyone experiences a “clogged” feeling at some point, there is a significant clinical difference between a temporary bout of sluggishness and a severe, chronic condition like Fecal Impaction.
Occasional Constipation (The Temporary Clog)
Occasional constipation is usually a short-term issue triggered by lifestyle changes. It typically lasts for a few days and resolves with simple home remedies.
-
Common Triggers: Traveling (vacation constipation), a low-fiber meal, slight dehydration, or a change in daily routine.
-
Symptoms: Hard stool that requires slight straining, a feeling of bloating, and fewer than three bowel movements a week.
-
Resolution: Usually responds quickly to increased water intake, a brisk walk, or a single dose of over-the-counter fiber.
Severe or Chronic Constipation (The Warning Zone)
Severe constipation, often termed Chronic Idiopathic Constipation (CIC), is a long-term condition defined by symptoms lasting for three months or more. According to the American College of Gastroenterology, this condition requires medical intervention because lifestyle changes alone often fail to provide relief.
-
Key Indicators: Consistent straining, the need for manual maneuvers to pass stool, and a persistent sensation of incomplete evacuation.
-
The Risk of Fecal Impaction: If severe constipation is left untreated, it can progress to Fecal Impaction, where a large, hard mass of stool becomes stuck in the rectum. This is a medical emergency that can cause intestinal obstruction.
Quick Comparison: Occasional vs. Severe
| Feature | Occasional Constipation | Severe/Chronic Constipation |
| Duration | A few days. | 3 months or longer. |
| Frequency | Rare or linked to a specific event. | Occurs consistently every week. |
| Pain Level | Mild bloating or discomfort. | Intense abdominal pain and cramping. |
| Response | Resolves with water/fiber. | Often requires laxatives or enemas. |
| Stool Type | Hard but manageable. | Stone-like (Type 1 on Bristol Scale). |
Understanding Your Results: The Bristol Stool Chart
The Bristol Stool Chart is a medical tool designed to classify the form of human faeces into seven categories. It helps you understand how long stool has spent in your colon.
Red Flags: When Occasional Becomes Severe
While most constipation cases resolve with home remedies, you should not ignore certain symptoms. While most cases of constipation are harmless and resolve with lifestyle changes, certain symptoms indicate a deeper medical emergency. According to the American College of Gastroenterology, if your constipation is accompanied by these “Red Flags,” you should seek professional medical advice immediately:
-
-
Intense Abdominal Pain: Sharp, stabbing, or persistent cramping that prevents you from standing straight.
-
Rectal Bleeding: Bright red blood on toilet paper or dark, tarry stools, which can indicate internal bleeding or fissures.
-
Inability to Pass Gas: If you are constipated and cannot even pass gas, it may signal a complete bowel obstruction.
-
Vomiting and Nausea: This often happens when waste is “backed up” in the digestive tract, a sign of severe fecal impaction.
-
Unexplained Weight Loss: Chronic constipation combined with losing weight without effort requires a clinical screening.
-
Fever and Weakness: These symptoms, alongside constipation, could indicate an infection in the colon, such as diverticulitis.
-
THE TOILET TRENCHES — It is a scene played out in bathrooms across the world: the silent, frustrating, and often painful struggle of stool that is “stuck” at the exit but won’t come out. While often dismissed as a minor inconvenience, medical experts warn that excessive straining is inefficient and can lead to severe long-term complications.
But what do you do when you are in that moment of crisis? New medical guidelines and physiological data from leading institutions like the Cleveland Clinic offer a clear, step-by-step roadmap to stimulate an immediate bowel movement without causing harm to your body.
The Posture Revolution: Shift to a Squat
The single most significant barrier to passing stool is often not the stool itself, but the angle of your body. Modern toilets force a 90-degree sitting position that is anatomically unnatural for defecation.
-
The Science: A key muscle, the puborectalis, wraps around the rectum like a sling. When you sit at 90 degrees, this muscle remains partially contracted, “kinking” the rectum and choking off the passage.
-
The Data: Research published by Harvard Health Publishing confirms that elevating your knees changes the anorectal angle from 90 degrees to a more acute 35 degrees. This creates a “straight shot” for stool to exit.
-
The Action: DO NOT sit and strain. Instead, place a small stool or a stack of books under your feet. This aligns your body into a natural squatting position.
Abdominal Massage: The ‘I Love U’ Technique
When internal contractions (peristalsis) fail, external stimulation can help restart the process. This method is highly recommended by physical therapists specializing in digestive health.
The Technique: Perform a focused massage on your lower abdomen using the “I Love U” (ILU) method:
-
-
I: Use your fingertips to apply gentle pressure, moving down the left side of your abdomen.
-
L: Move across the top from right to left, then down the left side.
-
U: Start at the bottom right, move up, across to the left, and down.
-
-
The Data: This specific pattern follows the path of the large intestine, helping to push trapped gas and waste toward the rectal vault.
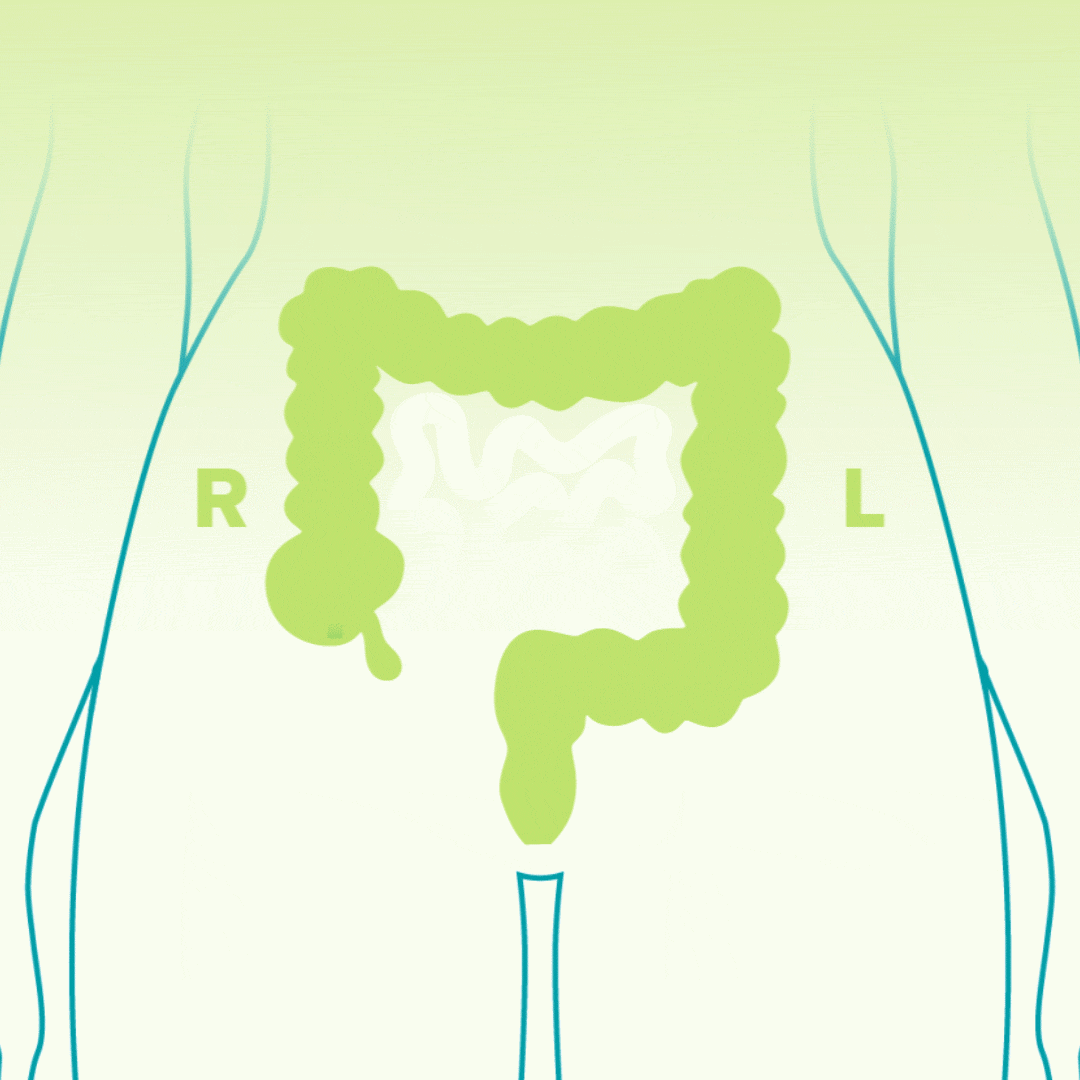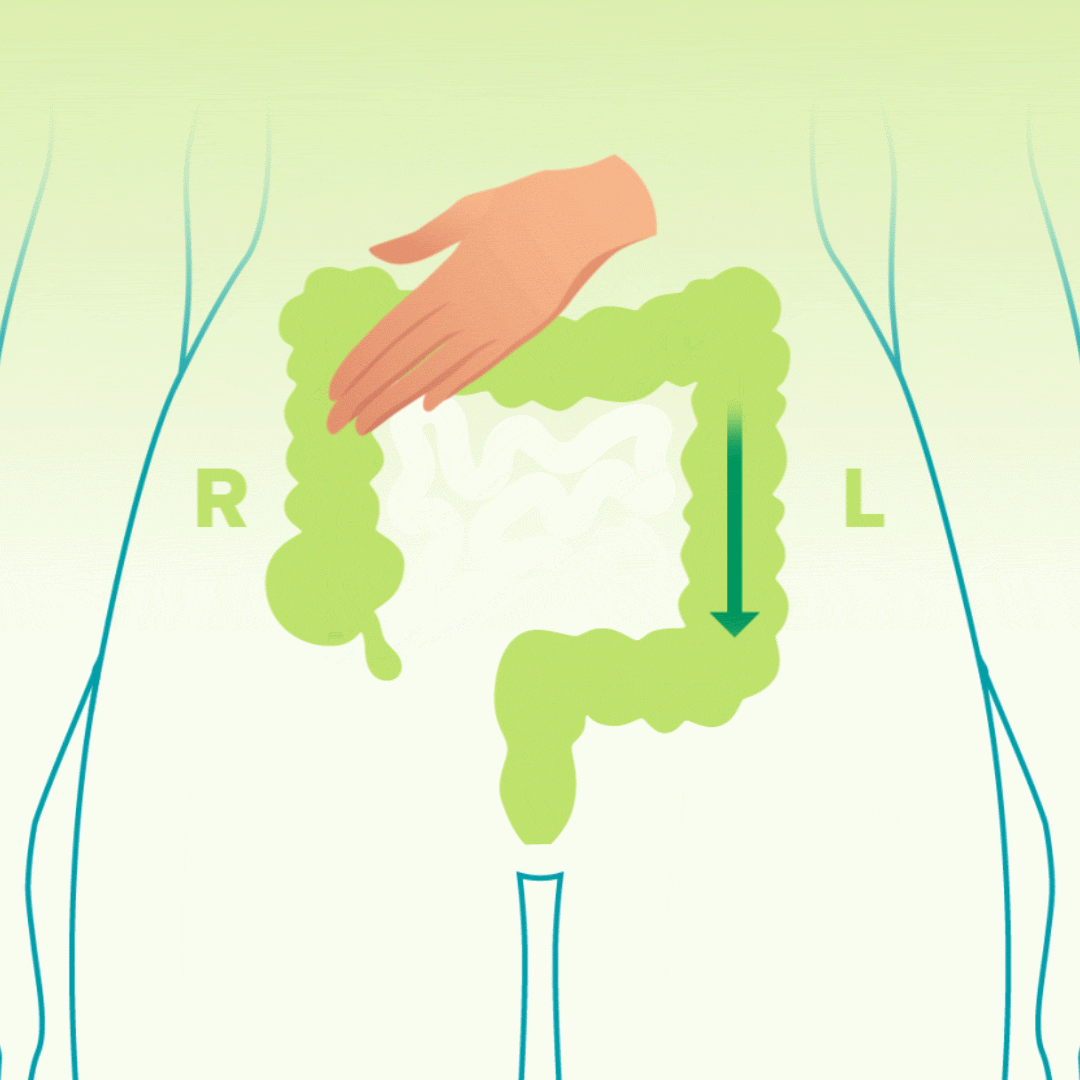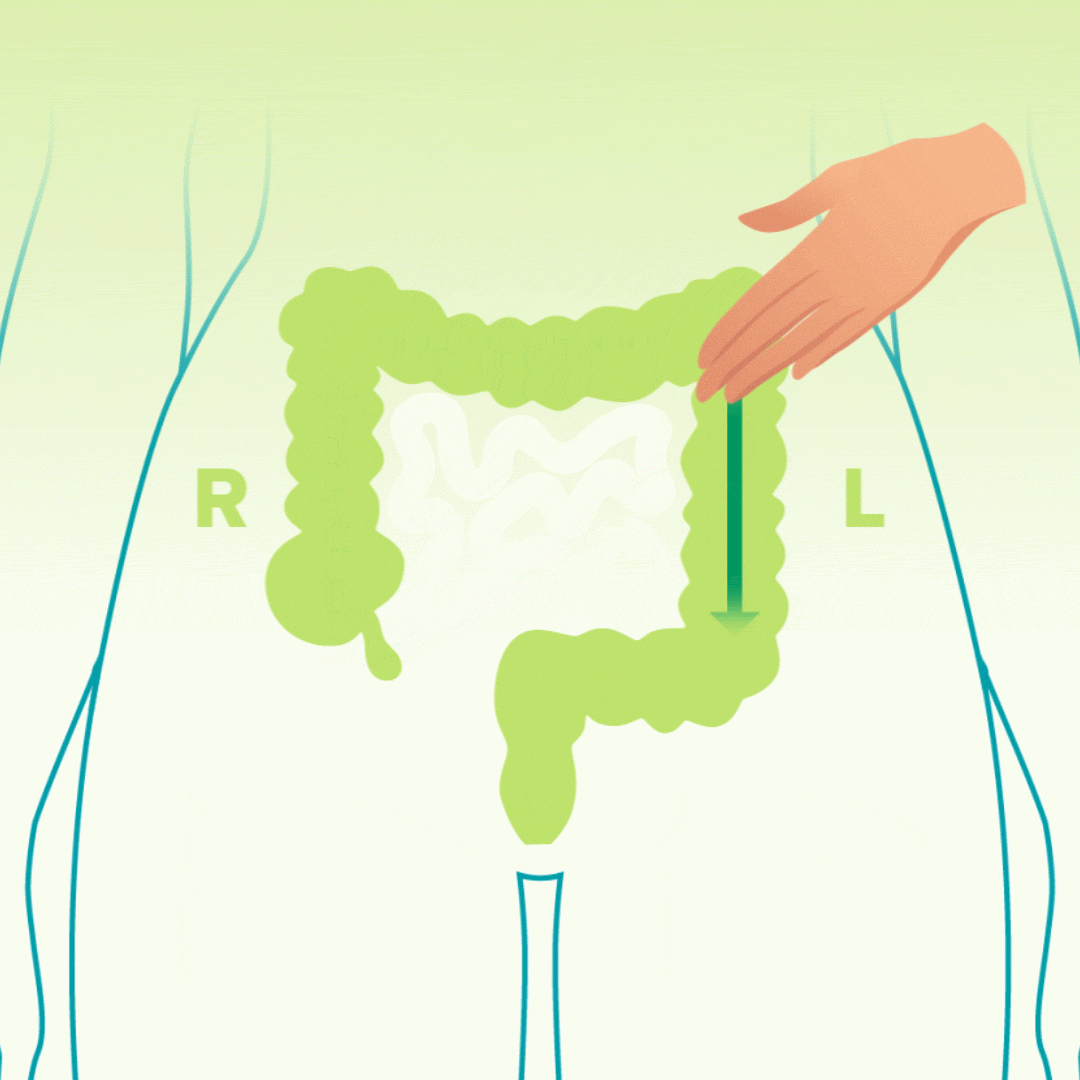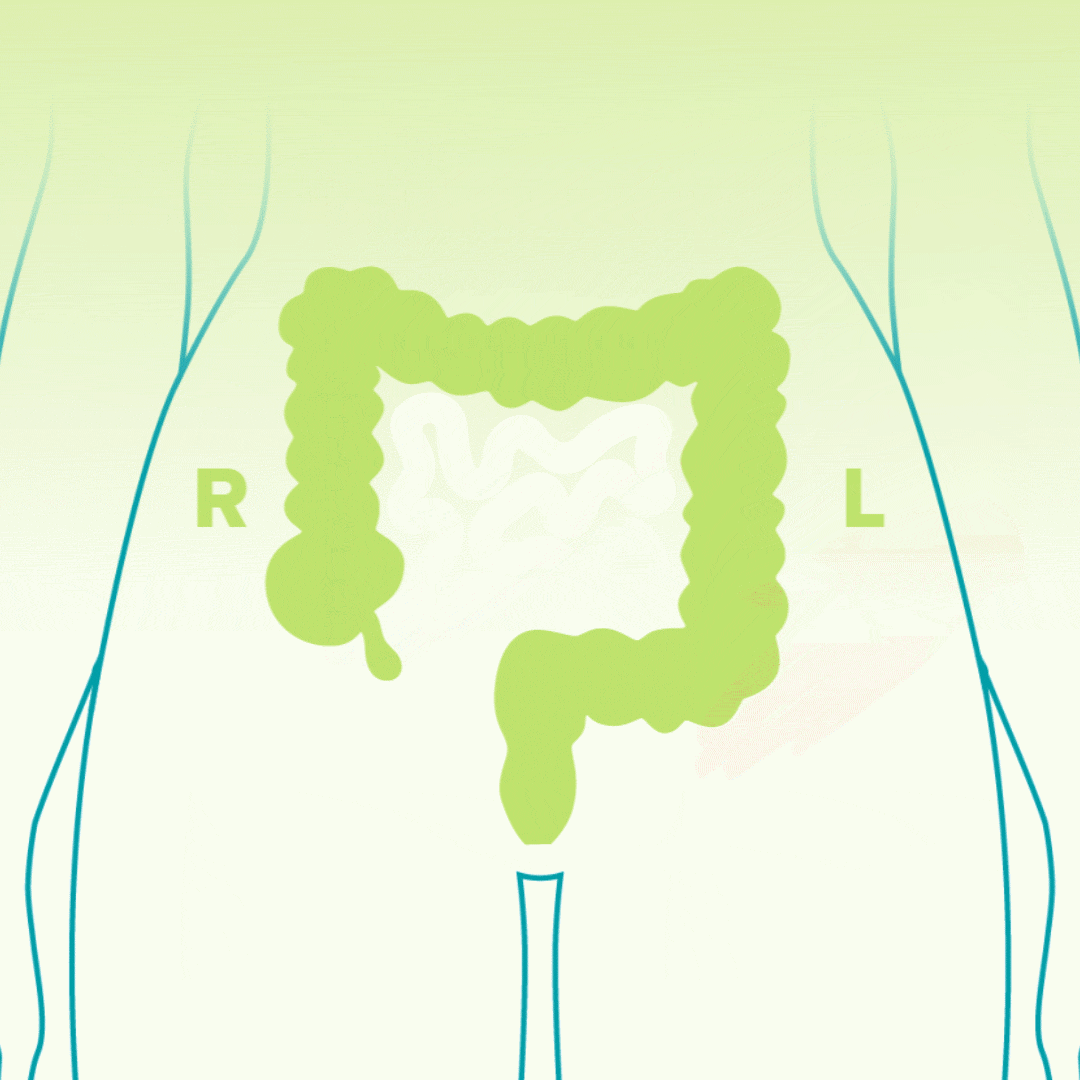
The ‘Blow Balloon’ Breathing Technique
Straining, or the Valsalva maneuver (holding your breath and pushing), is both ineffective and dangerous. It can cause blood pressure spikes and the development of painful hemorrhoids.
-
The Action: Instead of holding your breath, take a deep breath in and as you push gently, exhale slowly through your mouth as if you are blowing up a balloon.
-
The Science: This technique keeps your diaphragm relaxed and prevents the pelvic floor muscles from tensing up, allowing the stool to move naturally through the anal canal.
Warm Liquids to Trigger the Gastrocolic Reflex
Heat and certain compounds can jumpstart the muscles in your colon.
-
The Data: University of Michigan Health states that warm liquids can initiate the gastrocolic reflex. This is a physiological response where drinking or eating signals the colon to empty its contents.
-
The Action: Drink a large glass of warm water or a cup of black coffee. Coffee is significantly more effective than warm water at inducing colonic contractions.
The Emergency Option: Glycerin Suppository
If the stool is right at the exit but is too hard or large to pass, topical medication may be required to prevent tissue damage.
-
The Science: A Glycerin Suppository works as a lubricant and a mild irritant to stimulate the rectal muscles. It draws water into the rectum to soften the hard exterior of the stool.
-
The Data: Results typically occur within 15–30 minutes, providing a safer alternative to invasive enemas.
The Final Verdict: Know When to Stop
“When stool won’t pass, the goal must shift from force to synchronization,” suggest experts. If you have tried these steps for more than 20 minutes without success, stop. Leave the toilet, move around, and try again later. Forcing a bowel movement can cause serious injury, such as an anal fissure or rectal prolapse.
The correct toilet posture that makes bowel movements easier
THE ANATOMY OF RELIEF — For decades, modern society has been sitting on toilets at a 90-degree angle, unaware that this position is actually fighting against our own biology. If you’ve ever felt like your poop is “stuck” despite pushing hard, the culprit might not be your diet—it might be your posture.
According to groundbreaking research from Harvard Health Publishing and the Cleveland Clinic, the way we sit on a standard toilet effectively “kinks” the digestive tract, creating a physical barrier to waste elimination.
The Biological “Kink”: Why 90 Degrees Fails
Inside our pelvis, a muscle called the puborectalis acts like a rhythmic guardian of the rectum.
-
The Problem: When you sit upright at a 90-degree angle (the standard chair position), the puborectalis muscle only partially relaxes. It continues to pull on the rectum, creating a sharp bend known as the anorectal angle.
-
The Result: Attempting to poop in this position is like trying to run water through a kinked garden hose. You have to strain much harder to force the waste past that bend, which can lead to hemorrhoids and pelvic floor damage.
The 35-Degree Solution: The Power of Squatting
The human body was evolutionarily designed to squat. In a squatting position, our knees are brought up toward our chest, changing the internal geometry of the gut.
-
The Science: Elevating the knees above the hips shifts the body into a 35-degree angle. This position allows the puborectalis muscle to relax completely, straightening the anorectal angle.
-
The Data: A study published in the journal Digestive Diseases and Sciences found that individuals who used a squatting posture passed stool significantly faster and with far less straining than those who sat normally.

How to Achieve the Perfect Posture (Step-by-Step)
You don’t need to replace your toilet to get these benefits. You can modify your existing setup easily:
-
Use a Footstool: Place a small stool (like a “Squatty Potty” or a simple plastic step-stool) in front of your toilet.
-
Elevate Your Knees: Place your feet on the stool so that your knees are higher than your hips.
-
Lean Forward: Lean your torso slightly forward and rest your elbows on your knees. This further aligns the colon.
-
Straighten Your Spine: Keep your back straight rather than slouching to maintain internal alignment.
Why This Matters for Long-Term Health
Adopting the correct posture isn’t just about immediate relief. Consistent straining is a leading cause of:
-
Hemorrhoids: Swollen veins in the rectum caused by excessive pressure.
-
Anal Fissures: Small tears in the lining of the anus.
-
Pelvic Organ Prolapse: A serious condition where pelvic organs shift out of place due to chronic straining.
Foods, habits, and diets that naturally improve digestion
THE GUT REVOLUTION — While immediate relief techniques are vital during a crisis, true digestive freedom comes from long-term systemic changes. According to the World Gastroenterology Organisation, the secret to a “perfect” bowel movement lies not in a pill, but in a delicate balance of fiber, hydration, and biological timing.
“Your gut is like a high-performance engine,” says clinical data from Johns Hopkins Medicine. “If you give it the wrong fuel or never let it rest, it will eventually stall.”
The Fiber Foundation: Soluble vs. Insoluble
Not all fiber is created equal. To keep things moving, your body requires a strategic mix of two types:
-
Soluble Fiber: Found in oats, beans, and apples. It turns into a gel-like substance that softens the stool.
-
Insoluble Fiber: Found in whole grains and vegetables. It acts like a “broom,” adding bulk to the stool and sweeping it through the intestines.
-
The Data: A daily intake of 25–35 grams of fiber is the gold standard for preventing chronic constipation.
Hydration: The Lubricant of the Colon
Fiber without water is like a sponge without moisture—it becomes hard and difficult to move.
-
The Science: The large intestine’s primary job is to soak up water from waste. If you are dehydrated, the colon will pull too much water out, leaving your stool hard, dry, and “stuck.”
-
The Habit: Aim for 2–3 liters of water daily. A “Water-First” habit—drinking a large glass of room-temperature water immediately upon waking—triggers the gastrocolic reflex, preparing your system for its morning clearance.
Natural Probiotics and the Synbiotic to Help When Poop Stuck But Won’t Come Out
Your gut is home to trillions of bacteria (the microbiome) that play a critical role in breaking down food and regulating bowel movements. While most people focus on simple probiotics, clinical research now points toward a more powerful combination: Synbiotics.
-
The Probiotic Foundation: Incorporating fermented foods like Yogurt (Tok Doi), Kefir, or Sauerkraut introduces beneficial live bacteria (like Bifidobacterium and Lactobacillus) into your system.
-
The Science: According to studies in the American Journal of Clinical Nutrition, probiotics can significantly increase the number of weekly bowel movements and improve stool consistency by speeding up colonic transit time.
-
The Synbiotic Upgrade: A Synbiotic is the strategic combination of Probiotics (live beneficial bacteria) and Prebiotics (the specific fiber that feeds those bacteria).
-
Why Synbiotics are Superior for Constipation: Think of probiotics as “new seeds” for your gut and prebiotics as the “fertilizer.” When taken together, the beneficial bacteria are much more likely to survive the journey through your stomach acid and thrive in your colon.
-
The Result: Synbiotics have been shown to be a “game-changer” for chronic constipation. They not only add healthy bacteria but ensure they are active enough to stimulate the intestinal muscles to move waste forward efficiently.
How to Create a Synbiotic Meal at Home:
You don’t always need expensive supplements to get the synbiotic effect. Try these pairings:
-
Yogurt + Bananas/Oats: The live cultures in yogurt (probiotic) paired with the resistant starch in bananas or oats (prebiotic).
-
Kefir + Chia Seeds: The potent bacteria in kefir combined with the mucilaginous fiber of chia seeds creates a “super-sync” for your gut.
The “Circadian Rhythm” of Digestion
Your gut has its own internal clock. It is most active in the morning and slows down significantly at night.
-
The Habit: Establish a “Toilet Routine.” Try to sit on the toilet at the same time every morning (ideally 30 minutes after breakfast). Even if nothing happens, this consistent habit trains your brain and gut to work in sync.
-
The Rule: Avoid heavy, high-fat meals late at night. Late-night eating forces your digestive system to work when it should be repairing itself.
Movement: Gravity and Peristalsis
Exercise is a natural laxative. Physical activity increases blood flow to the GI tract and stimulates the smooth muscles that push waste forward.
-
The Data: Just 20 minutes of brisk walking daily can significantly reduce the time it takes for food to move through the large intestine.
Quick Checklist: The “No-Stall” Diet
To keep your digestion seamless, include these “Super-movers” in your weekly meal plan:
-
Prunes (Alubokhara): Nature’s most famous laxative, rich in sorbitol.
-
Chia Seeds: Capable of holding 12x their weight in water, adding perfect bulk.
-
Magnesium-Rich Greens: Spinach and kale help relax the intestinal muscles.
-
Papaya: Contains papain, an enzyme that specifically helps break down tough proteins.
Safe laxatives and natural remedies, including proper dosages and side effects
THE PHARMACOLOGICAL BALANCE — When lifestyle changes like hydration and fiber aren’t enough to break a severe blockage, laxatives become a necessary tool. However, the American Gastroenterological Association (AGA) warns that “laxative abuse” or choosing the wrong type can lead to dependency and a “lazy bowel.”
Understanding the different categories of laxatives—and their specific dosages—is the key to achieving relief without damaging your digestive system.
Osmotic Laxatives (The Safest Daily Option)
Osmotic laxatives are generally considered the first line of defense for chronic constipation because they don’t force the bowel to contract; they simply manage water.
-
How they work: They draw water from surrounding tissues into the colon, softening the stool and making it easier to pass.
-
Common Types: Polyethylene Glycol (Miralax) and Magnesium Hydroxide (Milk of Magnesia).
-
Proper Dosage: * Polyethylene Glycol: Typically 17g of powder dissolved in 4–8 oz of liquid once daily.
-
Side Effects: Bloating, gas, or mild abdominal cramping.
-
Expert Verdict: Safe for long-term use under medical supervision as they are not habit-forming.
Bulk-Forming Laxatives (Natural Fiber Supplements)
These are essentially concentrated fiber. They are the closest thing to a natural diet-based solution.
-
Common Types: Psyllium Husk (Ispaghula/Isabgol), Methylcellulose.
-
Proper Dosage: * Psyllium Husk: 1 tablespoon mixed thoroughly in a full glass of water, 1–3 times daily.
-
The Critical Rule: You must drink at least 8 oz of water with every dose. Without water, these can actually cause a physical blockage (impaction).
-
Side Effects: Initial bloating or gas as the gut microbiome adjusts.
Stimulant Laxatives (The Emergency “Push”)
These are more aggressive and should be used sparingly for “emergency” relief only.
-
How they work: They irritate the lining of the bowel, forcing the muscles to contract and push stool out.
-
Common Types: Senna (Sonamukhi), Bisacodyl (Dulcolax).
-
Proper Dosage: * Senna: Typically 8.6 mg to 17.2 mg once daily (usually at bedtime).
-
Side Effects: Sharp stomach cramps, diarrhea, and electrolyte imbalance.
-
Warning: Long-term use (more than 7 days) can lead to “Laxative Dependency,” where the colon loses its ability to move on its own.
Natural “Kitchen” Remedies
Before reaching for a pill, many natural substances provide clinical-grade results.
-
Prune Juice (Alubokhara): Contains Sorbitol, a natural sugar alcohol that acts as an osmotic laxative.
-
Dosage: 4–8 oz in the morning.
-
-
Castor Oil: A potent stimulant.
-
Dosage: 15 ml on an empty stomach. (Note: Avoid during pregnancy).
-
-
Aloe Vera Juice: Contains anthraquinones that stimulate the gut.
-
Dosage: 2–4 oz daily.
-
Summary Table: Laxative Comparison at a Glance
| Type | Examples | Speed of Action | Safety Level |
| Bulk-Forming | Psyllium (Isabgol) | 12–72 hours | High (Daily) |
| Osmotic | Miralax / Milk of Magnesia | 6–48 hours | High (Safe) |
| Stimulant | Senna / Bisacodyl | 6–12 hours | Low (Short-term only) |
| Suppository | Glycerin | 15–30 mins | Medium (Immediate) |
Special advice for children, pregnant women, and older adults
THE VULNERABLE GUT — Constipation doesn’t affect everyone the same way. Children, pregnant women, and older adults face unique physiological challenges that require more than just a “one-size-fits-all” solution. According to the American College of Gastroenterology, treating these groups requires a delicate balance between safety and effectiveness.
Children: Breaking the “Withholding” Cycle
Pediatric constipation is often behavioral as much as it is physical.
-
The Challenge: Children often “withhold” or resist having a bowel movement if they have had one painful experience. This leads to a cycle where the stool becomes larger and harder.
-
The Advice: Focus on “P” fruits—Prunes, Pears, and Plums. Ensure they are drinking enough water throughout the school day.
-
The Habit: Establish a “Toilet Training” routine. Have the child sit on the toilet for 5–10 minutes after breakfast or dinner to take advantage of the body’s natural urge.
-
Warning: DO NOT give stimulant laxatives to children without a pediatrician’s prescription.
Pregnant Women: Managing the Progesterone Shift
Constipation affects nearly 40% of pregnant women at some point during their journey.
-
The Challenge: High levels of progesterone relax the intestinal muscles, slowing down the passage of food. Additionally, the growing uterus puts physical pressure on the colon.
-
The Advice: Stick to Bulk-forming agents like Psyllium Husk (Isabgol) as they are not absorbed into the bloodstream. Increasing daily walking and fiber intake is the safest first step.
-
The Critical Warning: Avoid Castor Oil, as it can stimulate uterine contractions and lead to premature labor. Always consult your OB-GYN before taking any over-the-counter laxatives.
Older Adults: Combatting the “Slowing” System
As we age, the digestive system naturally loses some of its muscle tone, and medications often complicate the issue.
-
The Challenge: Reduced mobility, lower fluid intake, and the side effects of medications (like those for blood pressure or pain) are primary drivers of constipation in seniors.
-
The Advice: Focus on Osmotic Laxatives (like Miralax), which are much gentler on the aging gut than stimulants.
-
The Habit: Since the sensation of thirst diminishes with age, older adults should follow a “Hydration Schedule”—drinking a small glass of water every 2 hours, regardless of whether they feel thirsty.
The Hidden Dangers: Complications of Long-Term Constipation
THE SILENT STRAIN — Ignoring chronic constipation isn’t just uncomfortable; it can lead to serious medical conditions that require surgery.
-
Hemorrhoids: Swollen veins in the anus caused by chronic straining.
-
Anal Fissures: Small, painful tears in the lining of the anus.
-
Fecal Impaction: When stool becomes so hard and dry that it gets physically stuck in the rectum, requiring manual removal by a doctor.
-
Rectal Prolapse: A condition where part of the large intestine slips out of the anus due to years of excessive pushing.
Red Flags: When to See a Doctor Immediately
THE WARNING SIGNS — While most cases can be managed at home, certain “Red Flag” symptoms indicate a more serious underlying issue, such as bowel obstruction or even colorectal cancer.
Seek medical attention if you experience:
-
Blood in Stool: Bright red or dark, tarry stools.
-
Unexplained Weight Loss: Losing weight without trying while being constipated.
-
Severe Abdominal Pain: Cramping that doesn’t go away after a bowel movement.
-
Thin, Pencil-like Stools: A sign of a potential blockage in the colon.
-
Inability to Pass Gas: Combined with vomiting and bloating, this could be a bowel obstruction.
The Final Verdict: Lifestyle Changes for Long-Term Prevention
THE PATH TO FREEDOM — To ensure you never have to revisit the “Toilet Trenches,” adopt these four foundational habits:
-
The Fiber Rule: Aim for 30g of fiber daily.
-
The Hydration Habit: Drink a glass of water every 2 hours.
-
The Morning Ritual: Wake up, drink warm water, and walk for 10 minutes.
-
Listen to Your Body: Never ignore the “urge.” Delaying a bowel movement makes the stool harder and more difficult to pass later.
Conclusion: Reclaiming Your Digestive Freedom
THE PATH FORWARD — Constipation is more than just a physical inconvenience; it is a sign that your body’s internal rhythm is out of sync. As we have explored in this guide, overcoming the “Toilet Trenches” requires a multi-faceted approach. By aligning your posture to the natural 35-degree angle, fueling your gut with powerful Synbiotics, and maintaining the delicate balance of fiber and hydration, you can transform your digestive health.
Remember, consistency is key. The lifestyle changes you implement today—whether it’s a 10-minute morning walk or a daily glass of water—are the foundations of a life free from straining and discomfort. You don’t have to suffer in silence; with the right science-backed tools, regular and effortless bowel movements can become your new normal.
Medical Disclaimer
PLEASE READ CAREFULLY: The information provided on ConstipationRelief.net is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment.
-
Consult Your Doctor: Always seek the advice of your physician or another qualified health provider with any questions you may have regarding a medical condition or before starting any new diet, exercise, or supplement regimen (including laxatives and synbiotics).
-
Emergency Signs: If you are experiencing severe pain, fever, or rectal bleeding, seek immediate medical attention.
-
Accuracy: While we strive to provide the most up-to-date and scientifically accurate data, medical research is constantly evolving. Do not disregard professional medical advice or delay seeking it because of something you have read on this website.
FAQ
Q1: Is it normal to have a bowel movement only three times a week? A: Yes. According to the Mayo Clinic, the “normal” frequency ranges from three times a day to three times a week. Constipation is generally defined as fewer than three movements per week, accompanied by straining or hard stools.
Q2: Can I become dependent on laxatives if I use them too often? A: It depends on the type. Stimulant laxatives (like Senna or Dulcolax) can cause dependency if used for more than seven consecutive days. However, Bulk-forming (Psyllium) and Osmotic (Miralax) laxatives are generally safe for longer-term use under medical supervision.
Q3: Does drinking coffee really help with constipation? A: For many people, yes. Coffee stimulates the muscles in your digestive system, a process known as peristalsis. However, coffee is also a diuretic; if you don’t drink enough water along with it, it could eventually lead to dehydration and harder stools.
Q4: Why does my constipation get worse when I travel? A: This is known as “Traveler’s Constipation.” It happens because your body’s Circadian Rhythm is disrupted, your diet changes, and you may be sitting for long periods. To prevent this, stick to your morning routine and stay hydrated during flights or long drives.
Q5: Are Synbiotics better than regular Probiotics for constipation? A: Clinical data suggests yes. While Probiotics add healthy bacteria, Synbiotics provide both the bacteria and the “food” (Prebiotics) they need to thrive. This combination significantly improves colonic transit time and stool consistency more effectively than probiotics alone.
Read more on our website:
Scientific Sources and References
To ensure the highest level of accuracy, this guide is based on data from the following institutions:
-
Harvard Health Publishing: The lowdown on laxatives
-
Johns Hopkins Medicine: Constipation: What You Need to Know
-
Cleveland Clinic: The Proper Way to Poop: Is Your Posture Correct?
-
National Institutes of Health (NIH): Treatment for Constipation
-
American Journal of Clinical Nutrition: Probiotics and Synbiotics for Constipation Relief
-
World Gastroenterology Organisation (WGO): Global Guidelines on Constipation Management









